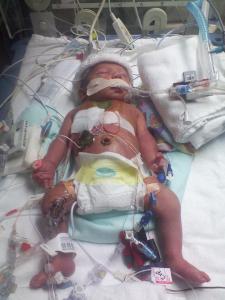
This is a picture of a baby similar to what we saw and to what our little Andrew will look like after his first Norwood open heart surgery. There were TONS of machines and tubes. It was just so real as soon as we were buzzed through the Cardiac Intensive Care Unit doors and going through the wash your hands to enter, wash your hands to leave, and seeing this huge wide open room and the babies separated by curtains. We had talked about and talked about this place, but seeing where he would be and this poor little baby similar to what he will look like was tough. The nurses in there kept talking about how much fight and strength these little babies have in them though. :)
We started out the day with another fetal echo and checking to make sure there were no changes to Andrew's heart and kind of confirming his diagnosis since the heart has gotten bigger. He still is in the same situation, same diagnosis...but the coarctation part (narrowing of the big artery that pumps blood out was not there this time. It was fine and no narrowing! So one less thing to worry over and one less thing in surgery to have to go in and fix (aside from the normal procedure)!
We talked with a cardiologist we weren't supposed to see today and she was too negative for my taste. She immediately started spouting high mortality rates with HLHS and that even if they have surgery and transplants it's not a permanent fix. She then went immediately into comfort care and went on and on about it and they offer you people and services of those that can talk to you that's been through it... (Comfort Care is just sending your baby home to slowly die on his own without fixing anything). Some people choose this option and it is in no place for me to say anything about that, but my son is coming into this world with a fighting chance and mommy and daddy are going to do any and everything we can to fight right along with him. So we pretty much shut down on her after that. I don't need someone telling me he has the worst CHD there is and all that mess. I'm aware of how serious it is, but I am also aware of how successful surgeries are.
During the Sibley Heart Center Tour we were taken to the floor where he would be until he went home in his own private room. He will have his own crib and there is a couch that turns into a bed and it has a shower in the room. This is where Shaun and I would be able to stay with him at all times and sleep if we want.
In the CICU that I mentioned first no one under 12 (including sisters) will be able to come see him. :( Also no one that is sick or even has a runny nose. Heart babies can get sick VERY easily. Also only 2 visitors at a time in the CICU. We will not be able to stay with him there (sleeping etc) but it is 24/7 access for mom and dad to come in and check on him there. They have a few times that everyone has to clear out (during rounds for confidentiality reasons since the room is one huge open room, but they will come get us when the surgeon or cardiologist come to Andrew and we will get to be a part of that). The expected stay is 7-10 days here (CICU) and then 2-3 weeks in the private room. Of course it will vary for each baby/case.
When he moves to his own room they will be doing constant teaching in there (for Shaun and I) and we will go through a discharge class and be sent home with any and everything we need to know to care for Andrew. The nurse that gave us the tour today said that feeding and getting the right amount of calories and weight gain is the key issue after surgery and before released from the hospital. She also said heart babies have really bad reflux most times. She did say they will have everything we need there for him and we can opt to bring his own things and clothes if we like for a homey feeling. She also said pictures and things can be hung in his room and on the walls in the CICU or the windows of his little bed rather. So we are going to get busy doing some projects for brother since the girls wont be able to see him for the first few weeks once he's in the CICU.
The surgeon was changed today on us, but he has been assigned, so he is the one doing Andrew's procedures. His name is Dr. Kogon. He said getting him through the first surgery is the vigorous part because it's the biggest surgery, but after the first surgery his survival rate goes to 87%. He said they like to say high 90's because that's what they experience there, but they like to say 87 instead.
He said after his first surgery he's still going to be in a very fragile stage. The second procedure is expected around 6 months and the third open heart surgery is around 3 years of age. After the first procedure the concerns could be complications from surgery (the shunt put in giving or something clogging, or since the right side does all the work for both sides of the heart since the left side isn't working or there that the right side after surgery could pump too little or too much to the lungs or to the body. They keep a close eye on them though and so will we and we will be well educated on what to look for at home.
SO ... A lot to take in, but it feels better to have a plan started. We go back in 5-6 weeks (34 weeks gestation for one last echo and then a confirmed/planned induction down at Grady in one of the last two weeks of July, or earlier if they think he needs surgery or whatever immediately). The only concern they really have with HLHS babies before due date time or induction time is the main hole that's open that they need to stay open getting smaller and right now his looks good. That's all for now. I'm wore out and have not been home since Wednesday morning really. Keep praying for our little Andrew! Thank you
We started out the day with another fetal echo and checking to make sure there were no changes to Andrew's heart and kind of confirming his diagnosis since the heart has gotten bigger. He still is in the same situation, same diagnosis...but the coarctation part (narrowing of the big artery that pumps blood out was not there this time. It was fine and no narrowing! So one less thing to worry over and one less thing in surgery to have to go in and fix (aside from the normal procedure)!
We talked with a cardiologist we weren't supposed to see today and she was too negative for my taste. She immediately started spouting high mortality rates with HLHS and that even if they have surgery and transplants it's not a permanent fix. She then went immediately into comfort care and went on and on about it and they offer you people and services of those that can talk to you that's been through it... (Comfort Care is just sending your baby home to slowly die on his own without fixing anything). Some people choose this option and it is in no place for me to say anything about that, but my son is coming into this world with a fighting chance and mommy and daddy are going to do any and everything we can to fight right along with him. So we pretty much shut down on her after that. I don't need someone telling me he has the worst CHD there is and all that mess. I'm aware of how serious it is, but I am also aware of how successful surgeries are.
During the Sibley Heart Center Tour we were taken to the floor where he would be until he went home in his own private room. He will have his own crib and there is a couch that turns into a bed and it has a shower in the room. This is where Shaun and I would be able to stay with him at all times and sleep if we want.
In the CICU that I mentioned first no one under 12 (including sisters) will be able to come see him. :( Also no one that is sick or even has a runny nose. Heart babies can get sick VERY easily. Also only 2 visitors at a time in the CICU. We will not be able to stay with him there (sleeping etc) but it is 24/7 access for mom and dad to come in and check on him there. They have a few times that everyone has to clear out (during rounds for confidentiality reasons since the room is one huge open room, but they will come get us when the surgeon or cardiologist come to Andrew and we will get to be a part of that). The expected stay is 7-10 days here (CICU) and then 2-3 weeks in the private room. Of course it will vary for each baby/case.
When he moves to his own room they will be doing constant teaching in there (for Shaun and I) and we will go through a discharge class and be sent home with any and everything we need to know to care for Andrew. The nurse that gave us the tour today said that feeding and getting the right amount of calories and weight gain is the key issue after surgery and before released from the hospital. She also said heart babies have really bad reflux most times. She did say they will have everything we need there for him and we can opt to bring his own things and clothes if we like for a homey feeling. She also said pictures and things can be hung in his room and on the walls in the CICU or the windows of his little bed rather. So we are going to get busy doing some projects for brother since the girls wont be able to see him for the first few weeks once he's in the CICU.
The surgeon was changed today on us, but he has been assigned, so he is the one doing Andrew's procedures. His name is Dr. Kogon. He said getting him through the first surgery is the vigorous part because it's the biggest surgery, but after the first surgery his survival rate goes to 87%. He said they like to say high 90's because that's what they experience there, but they like to say 87 instead.
He said after his first surgery he's still going to be in a very fragile stage. The second procedure is expected around 6 months and the third open heart surgery is around 3 years of age. After the first procedure the concerns could be complications from surgery (the shunt put in giving or something clogging, or since the right side does all the work for both sides of the heart since the left side isn't working or there that the right side after surgery could pump too little or too much to the lungs or to the body. They keep a close eye on them though and so will we and we will be well educated on what to look for at home.
SO ... A lot to take in, but it feels better to have a plan started. We go back in 5-6 weeks (34 weeks gestation for one last echo and then a confirmed/planned induction down at Grady in one of the last two weeks of July, or earlier if they think he needs surgery or whatever immediately). The only concern they really have with HLHS babies before due date time or induction time is the main hole that's open that they need to stay open getting smaller and right now his looks good. That's all for now. I'm wore out and have not been home since Wednesday morning really. Keep praying for our little Andrew! Thank you


 RSS Feed
RSS Feed
